Comedy King Dolphy Passes Away At 83
Dolphy, dubbed the country’s “King of Comedy,”whose body of work on stage, movies and television mirrors the history of Philippine entertainment, died on Tuesday night. He was 83. With his lean physique and humble demeanor, Dolphy’s memorable characters, notably as the down-on-his-luck family man John Puruntong in the long-running sitcom “John and Marsha,” effectively captured the travails of the common Filipino who is able to find humor even in the direst situations.
Dolphy died after a five-year battle with chronic obstructive pulmonary disease (COPD), according to his long-time partner, actress and singer Zsa Zsa Padilla. "We would like to inform the public that Mr. Rodolfo 'Dolphy' Quizon, passed away today, at 8:34 p.m. due to multiple organ failure, secondary to complications brought about by severe pneumonia, chronic obstructive pulmonary disease and acute renal failure," the Makati Medical Center said in a statement.
"We join the entire Filipino Community in praying for the soul of Mr. Quizon and his dearly beloved family and friends. To the Quizon Family, we extend our deepest condolences," the hospital said.
HEALTH FACTS
Multiple Organ Dysfunction Syndrome (MODS), previously known
as multiple organ failure (MOF) or multisystem organ failure (MSOF), is altered
organ function in an acutely ill patient requiring medical intervention to
achieve homeostasis. The use of "multiple organ failure" or
"multisystem organ failure" should be avoided since that phrase was
based upon physiological parameters to determine whether or not a particular
organ was failing
Streptococcus pneumoniae, a gram-positive bacteria, is the
most common cause of community-acquired pneumonia. It is a common cause of
septic shock with multiple organ dysfunction syndrome (MODS) resulting in
significant mortality. Gram-positive mouse models of sepsis with MODS are required
to examine mechanisms of immune responses in severe sepsis.
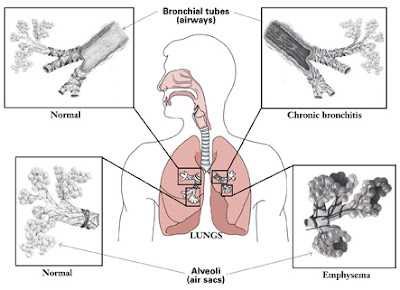
Chronic Obstructive Pulmonary Disease (COPD) is comprised primarily of three related conditions - chronic bronchitis, chronic asthma, and emphysema. In each condition there is chronic obstruction of the flow of air through the airways and out of the lungs, and the obstruction generally is permanent and may be progressive over time.
While asthma features obstruction to the flow of air out of the lungs, usually, the obstruction is reversible. Between "attacks" of asthma the flow of air through the airways typically is normal. These patients do not have COPD. However, if asthma is left untreated, the chronic inflammation associated with this disease can cause the airway obstruction to become fixed. That is, between attacks, the asthmatic patient may then have abnormal air flow. This process is referred to as lung remodeling. These asthma patients with a fixed component of airway obstruction are also considered to have COPD.
Often patients with COPD are labeled by the symptoms they are having at the time of an exacerbation of their disease. For instance, if they present with mostly shortness of breath, they may be referred to as emphysema patients. While if they have mostly cough and mucus production, they are referred to as having chronic bronchitis. In reality, it is better to refer to these patients as having COPD since they can present with a variety of lung symptoms.
There is frequent overlap among COPD patients. Thus, patients with emphysema may have some of the characteristics of chronic bronchitis and chronic asthma and vice a versa.
In general, symptoms of COPD don't appear until significant lung damage has occurred, and they usually worsen over time. People with COPD are also likely to experience episodes called exacerbations when their symptoms suddenly get much worse.
Signs and symptoms of COPD can vary, depending on which lung disease is most prominent. Most people have more than one of these signs and symptoms at the same time.
- Shortness of breath
- Wheezing
- Chest tightness
- Chronic cough
Acute kidney injury (AKI), previously called acute renal
failure (ARF), is a rapid loss of kidney function. Its causes are numerous and
include low blood volume from any cause, exposure to substances harmful to the
kidney, and obstruction of the urinary tract. AKI is diagnosed on the basis of
characteristic laboratory findings, such as elevated blood urea nitrogen and
creatinine, or inability of the kidneys to produce sufficient amounts of urine.
AKI may lead to a number of complications, including metabolic acidosis, high
potassium levels, uremia, changes in body fluid balance, and effects to other
organ systems. Management includes supportive care, such as renal replacement
therapy, as well as treatment of the underlying disorder.
The symptoms of acute kidney injury result from the various
disturbances of kidney function that are associated with the disease.
Accumulation of urea and other nitrogen-containing substances in the
bloodstream lead to a number of symptoms, such as fatigue, loss of appetite, headache,
nausea and vomiting. Marked increases in the potassium level can lead to
irregularities in the heartbeat, which can be severe and life-threatening.
Fluid balance is frequently affected, though hypertension is rare.
Pain in the flanks may be encountered in some conditions
(such as thrombosis of the renal blood vessels or inflammation of the kidney);
this is the result of stretching of the fibrous tissue capsule surrounding the
kidney. If the kidney injury is the result of dehydration, there may be thirst
as well as evidence of fluid depletion on physical examination.Physical
examination may also provide other clues as to the underlying cause of the
kidney problem, such as a rash in interstitial nephritis and a palpable
bladder.
Finally, inability to excrete sufficient fluid from the body
can cause accumulation of fluid in the limbs (peripheral edema) and the lungs
(pulmonary edema), as well as cardiac tamponade as a result of fluid effusions.
Source: www.wikipedia.com / www.abs-cbnnews.com